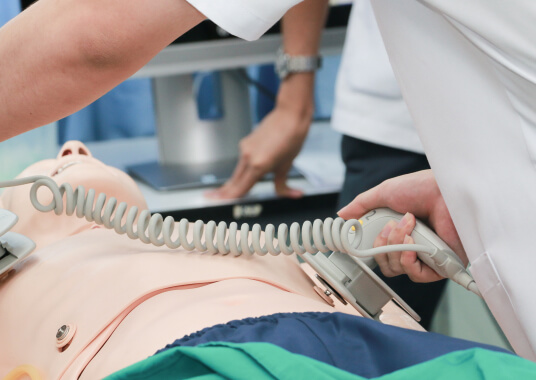
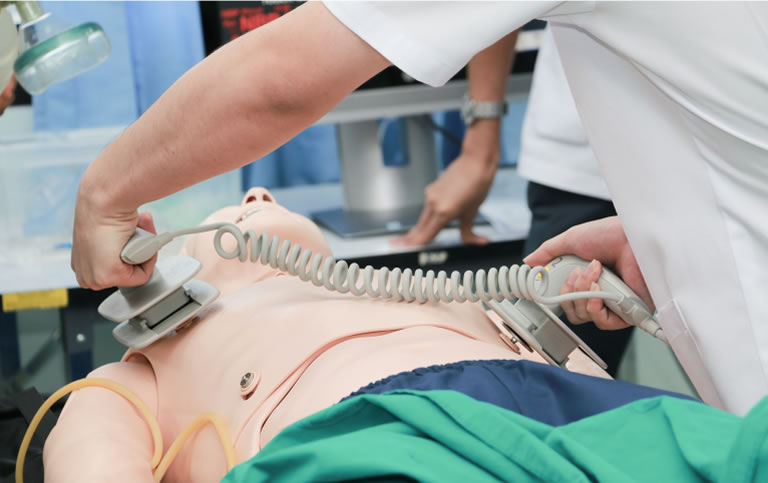
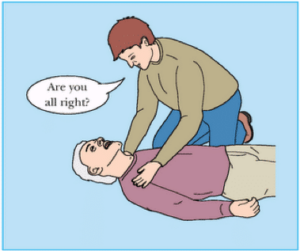
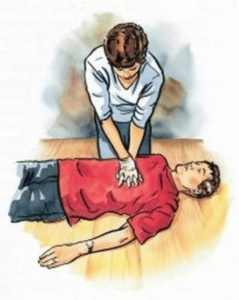
Basic life support is the initial response to a cardiac arrest and focuses on CPR and defibrillation. Advanced IV administration of drugs or advanced airway is not needed in BLS survey.
BLS has these components: Airway (A), Breathing (B), Chest compressions (C) and Defibrillation (D). The goal of BLS is to reinstate circulation, oxygenation and ventilation by focusing on CPR and defibrillation until the return of spontaneous circulation (ROSC). Before starting CPR,
The following is the Basic Life Support Algorithm:
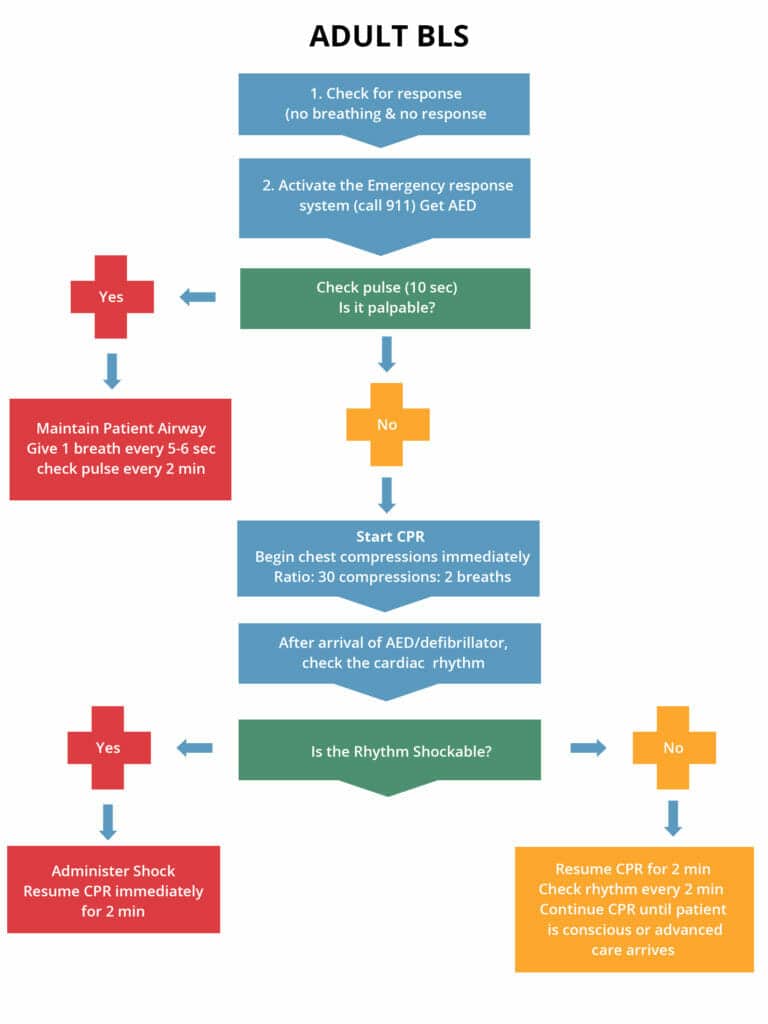
A Brief On ACLS
Once the
BLS primary survey is conducted the patient is then moved to the next level of care which is the ACLS. Advanced Cardiac Life Support is used after ineffective BLS or if there is a conscious patient who needs advance medical attention. The main goal of
ACLS is to provide a more invasive procedure, advance assessment, proper management techniques, and differential diagnosis for the overall health of the patient.
ACLS Survey
| ASSESSMENT |
TECHNIQUE/ACTION |
Airway
- Is the airway patent?
- Is an advanced airway indicated?
- Is placement of advanced airway confirmed?
- Check if placement of airway is secure and check continuously
|
In an unconscious patient use the following to sustain airway patency:
- Head tilt-chin life
- Oropharyngeal airway (OPA)
- Nasopharyngeal airway (NPA)
If needed use the following advanced airway management:
- Laryngeal mask airway
- Laryngeal tube
- Esophageal-tracheal tube
- Endotracheal tube
To minimize interruptions of CPR and ventilation, insert airway quickly
Ensure advanced airway is placed correctly by:
- Physical examination
- Quantitative waveform capnography
Ensure the device is stabilized
Use quantitative waveform capnography to
Ensure monitor is placed correctly |
Breathing
- Is oxygenation and ventilation sufficient?
- Is there continuous monitoring of quantitative waveform capnography and oxyhemoglobin saturation?
|
Give supplementary oxygen when needed:
- Patients who are in cardiac arrest, provide 100% oxygen
- For everyone else, titrate oxygen administration to achieve oxygen saturation values of at least 94% (always confirm with pulse oximetry)
- Monitor ventilation and oxygenation by
- Clinical criteria (chest rise and cyanosis)
- Quantitative waveform capnograpy
- Oxygen saturation
|
Circulation
- Are you providing adequate chest compressions?
- Cardiac rhythm?
- Is defibrillation or cadioversion needed?
- IV/IO access obtained?
- Is the patient with a pulse unstable?
- Medications needed?
- Need IV fluids?
|
- Monitor quality CPR
- Attach monitor/defibrillator for arrhythmias or cardiac arrest rhythms
- Give defibrillation/cardioversion
- Get IV/IO access
- Administer appropriate drugs
- Provide IV/IO fluids if needed
|
Differential Diagnosis
- What caused the symptoms or arrest?
- What are the reversible causes and can it be treated?
|
- Look for and treat any reversible issues
- Remember the H’s & T’s
THE H’S:
- Hypovolemia, Hypoxia, Hydrogen ion (acidosis), Hyper/hypokalemia, Hypothermia
THE T’S:
- Toxins, Tamponade (cardiac), Tension pneumothorax, Thrombosis (coronary or pulmonary)
|
Learning Outcomes:
You have completed Course II. Now you should be able to:
- Understand the basic BLS and ACLS survey
- Explain the BLS survey in detail
- Explain what initial steps you should take during a cardiac arrest situation